The Metabolic Link: How ADHD Intersects with Insulin Resistance and Inflammation
Attention-Deficit/Hyperactivity Disorder (ADHD) is increasingly recognized as more than just a neurobehavioral condition. Compelling evidence from psychiatric and metabolic journals demonstrates a strong, often bidirectional, biological link between ADHD and serious physical health risks, primarily components of the Metabolic Syndrome (MetS).
1. The Clinical Connection: High-Risk Comorbidity
Individuals with ADHD—across the lifespan—face a statistically higher risk for developing several key conditions:
Obesity and Diabetes: ADHD is an independent risk factor for both obesity and Type 2 Diabetes Mellitus (T2DM).
Insulin Resistance (IR): IR, where the body's cells don't respond properly to insulin, is a common feature observed in adult and adolescent ADHD populations, often leading to poorer glycemic control.
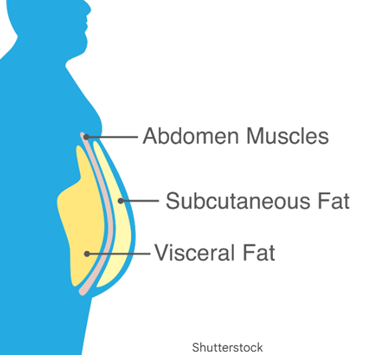
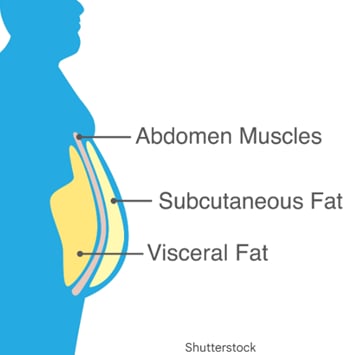
Visceral Fat Accumulation: Crucially, recent studies show that individuals with ADHD and obesity tend to accumulate significantly greater visceral fat (fat stored around abdominal organs) than those who are obese without ADHD. This type of fat is highly inflammatory and directly drives metabolic disease.
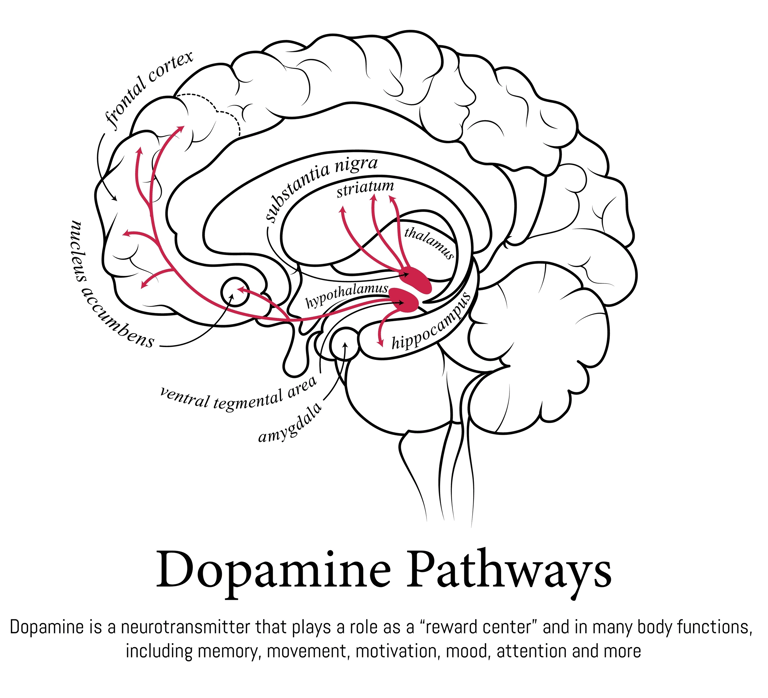
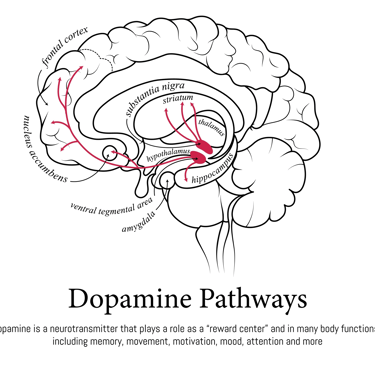
A. Dopamine Dysregulation and Hedonic Eating
The Problem: ADHD is characterized by dysregulation in the dopamine system, which governs attention, motivation, and—critically—reward processing.
The Mechanism: This can lead to impulsive and hedonic eating, where individuals seek out high-fat, high-sugar foods to compensate for low basal reward/dopamine levels. This pattern contributes directly to weight gain and metabolic strain.
B. Chronic Low-Grade Inflammation
The Bridge: Chronic, low-grade systemic inflammation acts as a key link. Visceral fat is a major source of inflammatory molecules.
The Effect: This inflammation disrupts the body's ability to use insulin effectively (driving insulin resistance) and is also theorized to contribute to neuroinflammation that can exacerbate or influence ADHD symptoms.
3. Clinical Takeaway
The growing body of research suggests that individuals with ADHD should be considered a high-risk group for cardiometabolic complications. Screening and management strategies must therefore address both the neurodevelopmental symptoms and the underlying metabolic health to improve long-term outcomes.
4. Citations and Reputable Sources
The information presented is supported by findings published in the following peer-reviewed journals and authoritative medical databases: